 Immediacy – treat them without delay and not wait until the wounded were all dealt with.Proximity – treat the casualties close to the front and within sound of the fighting. 
The following PIE principles were in place for the "not yet diagnosed nervous" (NYDN) cases: The World War II European Army rate of stress casualties of 1 in 10 (101:1,000) troops per annum is skewed downward from both its norm and peak by data by low rates during the last years of the war. Modern warfare embodies the principles of continuous operations with an expectation of higher combat stress casualties. In low-level conflicts, it can drop to 1:10 (or less). With intense fighting, it can be as high as 1:1. The ratio of stress casualties to battle casualties varies with the intensity of the fighting. The large proportion of World War I veterans in the European population meant that the symptoms were common to the culture. Soldiers were personally faulted for their mental breakdown rather than their war experience. Whether a person with shell-shock was considered "wounded" or "sick" depended on the circumstances. The nature of trench warfare meant that about 10% of the fighting soldiers were killed (compared to 4.5% during World War II) and the total proportion of troops who became casualties (killed or wounded) was about 57%. In World War I, shell shock was considered a psychiatric illness resulting from injury to the nerves during combat. Many reactions look like symptoms of mental illness (such as panic, extreme anxiety, depression, and hallucinations), but they are only transient reactions to the traumatic stress of combat and the cumulative stresses of military operations. This term can be applied to any stress reaction in the military unit environment. 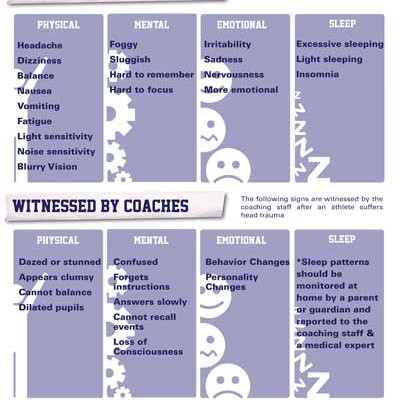
The US Army uses the term/initialism COSR (combat stress reaction) in official medical reports. Combat stress reaction is generally short-term and should not be confused with acute stress disorder, post-traumatic stress disorder, or other long-term disorders attributable to combat stress, although any of these may commence as a combat stress reaction. The most common symptoms are fatigue, slower reaction times, indecision, disconnection from one's surroundings, and the inability to prioritize. It is historically linked to shell shock and can sometimes precurse post-traumatic stress disorder.Ĭombat stress reaction is an acute reaction that includes a range of behaviors resulting from the stress of battle that decrease the combatant's fighting efficiency. Also known as "combat fatigue", "battle fatigue", or "battle neurosis", it has some overlap with the diagnosis of acute stress reaction used in civilian psychiatry. 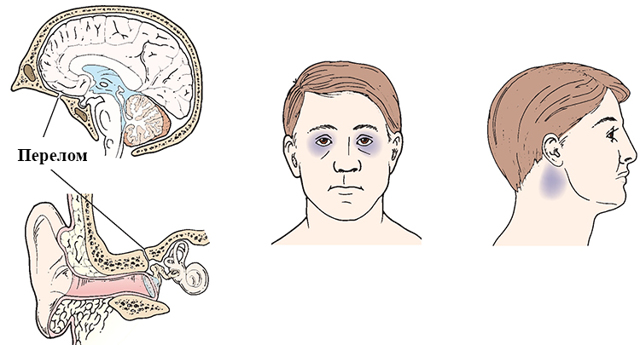
Miller, exhibits a " thousand-yard stare", an unfocused, despondent and weary gaze which is a frequent manifestation of "combat fatigue"Ĭombat stress reaction ( CSR) is acute behavioral disorganization as a direct result of the trauma of war. More rarely, allergies can also cause raccoon eyes, but the coloring is typically less prominent.A U.S. Although trauma is the most common cause of raccoon eyes, other conditions can also cause it, such as: Differential diagnosisĪ differential diagnosis is when doctors have to rule out conditions that have very similar symptoms. If head or facial swelling remains within a couple of days, then raccoon eyes may soon follow. It’s important to note that raccoon eyes may not develop immediately after an injury. 
A broken nose or broken cheekbones are other possible causes. BSF can occur from car accidents, falls, sports injuries, and other sources of head trauma.Īnother possible cause of raccoon eyes is the breaking of the thin bones that surround your eyes. When a fracture occurs, symptoms such as raccoon eyes may follow. The basal part of your skull is the bottom portion where the brain rests. Raccoon eyes is most often caused by a basal skull fracture (BSF). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
